Are you coughing frequently with purulent sputum? Know the signs of bronchiectasis
Author: Jin Jianmin, Chief Physician at Beijing Tongren Hospital, Capital Medical University.
Review: Zhang Haicheng, Chief Physician at Peking University People's Hospital.
Bronchiectasis is not the same as bronchiectatic disease; distinguishing between these concepts is the first step in understanding this respiratory condition.
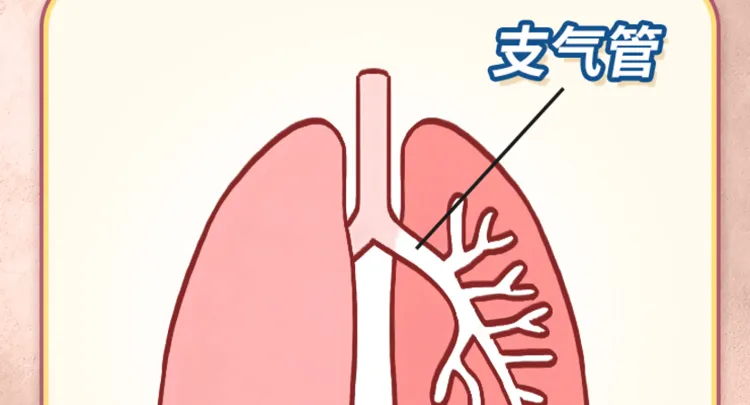
Bronchiectasis is an anatomical concept frequently encountered in CT reports. It indicates the dilation of the bronchial lumen beyond the normal diameter. Essentially, our trachea and bronchi can be likened to a tree, branching progressively finer. When various factors cause the lumens to widen from the small bronchi to the bronchi, this condition is termed bronchiectasis, signifying a change in the bronchial-pulmonary structure.
Bronchiectasis represents an independent primary disease. Patients diagnosed with bronchiectasis will invariably exhibit signs of bronchial dilation on a CT scan. However, bronchial dilation seen on a CT does not necessarily equate to a diagnosis of bronchiectasis. Several other conditions, such as pulmonary interstitial fibrosis with traction bronchiectasis and sequelae from pulmonary tuberculosis, can also produce bronchial dilation, resulting from an underlying primary condition rather than representing a distinct disease.
In clinical practice, physicians often refer to the term "bronchiectasis" generically. When patients inquire, "What disease do I have?" doctors might typically reply, "You have bronchiectasis." Here, the term "bronchiectasis" generally points towards the specific disease identified as "bronchiectasis."
Bronchiectasis is a chronic infectious respiratory disease primarily characterized by recurrent cough, prodigious amounts of purulent sputum production, and occasional hemoptysis. The key diagnostic criterion is the distinctive findings on high-resolution CT (HRCT) scans of the lungs. Currently, precise statistics regarding its incidence are scarce. International literature suggests that the incidence of bronchiectasis among American adults is approximately 52 per 100,000 individuals; however, this data may be outdated given the limited use of HRCT scans in the past. In China, bronchiectasis is not as frequently acknowledged as conditions like asthma or chronic obstructive pulmonary disease (COPD), leading to a lack of national incidence data.
The pathogenesis of bronchiectasis revolves around the interplay of bronchopulmonary infections and bronchial obstruction, resulting in a detrimental cycle.
Under typical physiological conditions, airway secretions are expelled effectively through mechanisms like ciliary movement. However, inflammation can trigger a marked increase in secretion volume. In cases where bronchial obstruction is present, normal expulsion of sputum is hindered, leading to accumulation in the bronchi. This buildup exacerbates airway obstruction, potentially inciting more intense airway inflammation and damaging supportive structures such as the smooth muscle and elastic fibers in the bronchial wall. The cycle of "infection-obstruction-reinfection" may recur, leading to the persistent and irreversible dilation of the bronchi, eventually culminating in bronchiectasis.
The causes of bronchiectasis can be classified into several categories:
First, bronchial-pulmonary infection stands as the primary cause. Infections from various pathogens induce inflammation, with the most predominant bacteria being Haemophilus influenzae, Klebsiella pneumoniae, and Pseudomonas aeruginosa. Among viruses, the measles virus is notably common; many individuals contract this illness during childhood, with potential progression to bronchiectasis in later life. Moreover, non-tuberculous mycobacterial infections represent another significant factor.
Second, bronchial obstruction contributes to the condition. For instance, an inhaled object causing airway blockage may lead to obstructive pneumonia in the lung tissue distal to the obstruction, resulting in inflammatory secretions that cannot be expelled, thereby contributing to localized bronchiectasis. Fortunately, these causes are generally removable; timely extraction of the foreign body can lead to improvement in associated bronchiectasis.
Additionally, disorders pertaining to ciliary motility in the airways constitute another possible cause. Normally, cilia within the airways move in a coordinated fashion to clear secretions. However, if there is a disturbance in ciliary motion, such as immobility or disorganized movement, secretions may accumulate, which exacerbates bronchiectasis. Conditions related to this disruption include primary ciliary dyskinesia, Kartagener syndrome, among others.
Lastly, hereditary disorders, including congenital abnormalities in bronchial wall development and α1-antitrypsin deficiency, may also lead to bronchiectasis.
Understanding these fundamental concepts aids patients and families in gaining a clearer perspective on the nature of bronchiectasis, distinguishing between the notions of "bronchiectasis" and "bronchiectasis disease." This understanding facilitates improved communication with healthcare providers about the condition and treatment alternatives, thus enhancing cooperation in management and treatment.
© 2025 Health Tribe.


