What is heartburn and how does it affect your health
Author: Li Haoyan, undergraduate student of Clinical Medicine, Class of 2024, Chongqing Medical University. Supervisor: Associate Professor Xu Lei from the Department of Immunology and Pathogen Biology at Chongqing Medical University, and Director Technician Zou Jingbo from the Volunteer Service Team for Health Science Popularization of the Red Cross in Yongchuan District, Chongqing (Zou's Science Garden), an expert from Science Popularization China. Review Expert: Wang Yang. Contribution Unit: Chongqing Microbiology Society. Statement: Except for original content and special notes, some images are sourced from the internet and are for non-commercial use only, serving as materials for popular science communication. Copyright belongs to the original authors. If there are any infringements, please contact for removal.
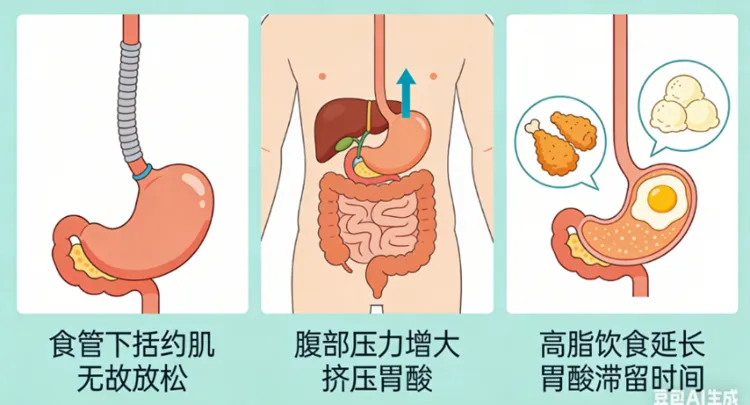
Title: What is heartburn and how does it affect your health. Introduction: Heartburn, caused by stomach acid irritating the esophagus, can be managed by adjusting diets and improving lifestyles. Keywords: ['Health', 'Digestion']. Many friends from the Sichuan and Chongqing regions may have had this experience: after finishing a meal and returning home, having cleaned up, you lie in bed feeling satisfied while scrolling through your phone. Suddenly, a burning sensation shoots up from the back of your chest, accompanied by a sour taste that rises in your throat. This distinctly sour experience often occurs after a spicy hot pot meal, and many friends refer to it as 'heartburn.' In fact, this sensation of 'burning in the heart' is often unrelated to the heart itself; rather, it is caused by an irritated stomach leading to reflux, which then stimulates the esophagus, causing it to become agitated. But why is it that when there are problems in the stomach, the first sensation of discomfort is felt in the chest? This can be attributed to our body's rather imprecise 'alert system.' The sensory nerves of the esophagus and the heart travel along the same signaling pathway to the brain. When stomach acid irritates the esophagus, the nerve signals return to the spinal cord, and the brain can easily get confused in its interpretation: 'A signal from the chest? That must be the heart!' Thus, a misunderstanding occurs. This phenomenon is medically referred to as referred pain—where the organ experiencing the issue and the location where the pain is felt are not the same. Therefore, the term 'heartburn' is a classic case of misnaming. It is not the heart that is burning; rather, it is the esophagus, that muscular tube measuring 25 centimeters that extends from the throat to the stomach. The 'heartburn' scene actually takes place here: at the junction between the esophagus and the stomach, there is a ring of special muscle known as the lower esophageal sphincter (LES). Under normal circumstances, it acts as a diligent security guard: food can go down, but nothing from the stomach should come back up. However, in some cases, this security guard may also fail: the lower esophageal sphincter 'takes a break' and relaxes. Sometimes this ring of muscle suddenly relaxes without reason for a few seconds, allowing stomach acid to reflux upwards. Bending over to pick something up after a big meal, wearing tight pants, being overweight, or being pregnant can increase abdominal pressure. This is similar to squeezing toothpaste, forcing stomach acid up into the esophagus. A high-fat diet and binge eating prolong the retention time of stomach acid, increasing the risk of acid reflux. Compared to the thick mucous barrier of the stomach wall, the esophageal mucosa is much more delicate. When this situation occurs, the hydrochloric acid in the stomach, mixed with a variety of digestive enzymes, backs up into the esophagus, compromising the esophageal mucosa and causing damage to the esophagus—this is the essence of heartburn. 'It's just acid reflux; just bear with it and it will pass'—this is the most dangerous mindset. Allowing the esophagus to be immersed in stomach acid for a long time leads to gradual consequences: esophagitis. The esophageal mucosa is repeatedly burned by acid, leading to erosion and ulcers. At this point, you may feel pain when swallowing, and even experience difficulty swallowing. Barrett's esophagus. Under prolonged stimulation, the normal cells in the lower part of the esophagus become 'desperate' and decide to mutate in a bid for survival, transforming into columnar epithelial cells resembling those in the intestine. Patients with this condition often face a higher risk of developing esophageal adenocarcinoma compared to the general population. Esophageal stricture or cancer. Repeated damage and repair can lead to scarring, causing the esophagus to narrow increasingly, making it difficult to even drink water. But there is also good news: gastroesophageal reflux disease can be controlled by adjusting lifestyle habits. Dietary habits: reduce high-fat, spicy, and acidic foods. Reduce the consumption of coffee, alcohol, and chocolate. Do not eat within three hours before bedtime. Sleep habits: do not lie down within 2-3 hours after eating. Raise the head of the bed appropriately. Body weight and clothing: weight loss, abdominal fat is the biggest enemy of LES, as it will continuously exert pressure upwards. Quit smoking; nicotine relaxes the sphincter muscles. Loose-fitting clothing; give up those tight-waisted pants and corsets. Gastroesophageal reflux disease may seem like just a 'slight discomfort,' but it is actually a distress signal from your body. Next time you face a spicy hot pot, remember that somewhat unreliable 'esophageal security guard,' LES. Treat it better: eat a little less and stand a bit longer, and your esophagus will be grateful. References: 1. Lynn, R.B., Mechanisms of esophageal pain. Am J Med, 1992. 92(5A): p. 11S–19S. 2. Chinese Medical Association Gastroenterology Branch Gastrointestinal Motility Group, et al. Guidelines for the Diagnosis and Treatment of Gastroesophageal Reflux Disease in China. Gastroenterology, 2023, 28(10): p. 597–607. 3. Tack, J. and J. E. Pandolfino, 'Pathophysiology of Gastroesophageal Reflux Disease.' Gastroenterology, 2018. 154(2): pp. 277–288. 4. Hvid-Jensen, F., et al. Incidence of adenocarcinoma among patients with Barrett's esophagus. N Engl J Med, 2011. 365(15): pp. 1375–83. 5. Ness-Jensen, E., et al., Lifestyle Intervention in Gastroesophageal Reflux Disease. Clinical Gastroenterology and Hepatology, 2016, 14(2): pp. 175–182.e1–3.
© 2025 Health Tribe.