Guidelines for Treating Lower Limb Arterial Disease at Home
Author: Wang Dandan, Head Nurse of the Endocrinology Department at the Air Force Specialty Medical Center. Chen Xia, Chief Nurse of the Cardiothoracic Surgery Department at the Air Force Specialty Medical Center. Review: Wang Liangchen, Associate Chief Physician of the Endocrinology Department at the Air Force Specialty Medical Center. Produced by: Popular Science China.
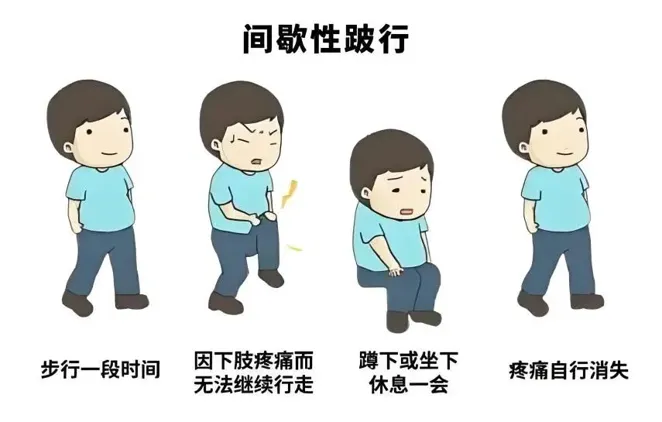
Title: Guidelines for Treating Lower Limb Arterial Disease at Home. Introduction: Lower limb arterial disease, caused by atherosclerosis, needs awareness and proper care to improve patient outcomes and health. Keywords: health, vascular health. What is peripheral arterial disease? Lower extremity arterial disease (LEAD) refers to the progressive narrowing or obstruction of the lumen of the arteries in the lower limbs caused by atherosclerosis, which leads to reduced blood flow to the lower extremities. This can result in symptoms such as lower limb ischemia, pain, and mobility issues. In severe cases, it can lead to amputation or even death. 2. Clinical Manifestations of LEAD. LEAD is often asymptomatic in the early stages; as the disease progresses, patients may experience intermittent claudication and resting pain. In the advanced stages, foot ulcers or gangrene may occur. If not treated promptly, the amputation rate can reach 20%, and the 5-year mortality rate can be as high as 50%. The typical signs mainly include coldness in the distal limbs, sensitivity to cold, numbness, and soreness; intermittent claudication; dry skin, thin skin, and shedding of fine hair, which are symptoms of muscle atrophy; thickened or slow-growing toenails; pale, flushed, or purplish skin; decreased or absent arterial pulse in the lower limbs; resting pain (patients often sit with their knees drawn up); and ulcers or gangrene in the affected limbs. Intermittent claudication refers to pain induced by exercise, often manifesting as heaviness, fatigue, distension, dull pain, cramping pain, or sharp pain in areas with insufficient blood supply during walking, or a pronounced sense of numbness in the extremities, which forces the patient to stop. After resting for a moment, the pain lessens, and this cycle repeats. This condition commonly occurs in the calf muscles but can also be found in some patients in the gluteal area. Illustration: Symptoms of Intermittent Claudication. 2. Interventional Therapy for LEAD (Limb-to-Energy Arterial Disease). Revascularization methods (referred to as intervention) are effective in reducing amputation rates and improving prognosis in the treatment of LEAD. Interventional therapy has advantages such as minimal invasiveness, quick recovery, and significant efficacy, making it a primary approach for treating LEAD. This includes procedures like percutaneous transluminal balloon angioplasty, stent implantation, and endovenous volume reduction. Illustration: Diagram of LEAD Interventional Therapy. Postoperative care for LEAD intervention treatment. 1. Positional Care. The '6-12-24' principle of supine positioning. After surgery, the patient should remain in a supine position, following the '6-12-24' principle. The puncture site should be compressed for 6-8 hours; the limb on the same side as the puncture site should remain in a straight position, with activity limited for 12 hours. For the first 24 hours post-surgery, the patient should restrict getting out of bed, and may only do so after the doctor removes the bandage. Buerger's disease. Patients with lower limb ulcers can perform dorsiflexion and plantarflexion exercises or Buerger exercises in bed 24 hours after surgery. 2. Care for the Affected Limb. It is necessary to observe changes in vital signs, check for any seepage of blood at the puncture site, and monitor for changes in skin color of the lower limbs. If there is any seepage of blood at the puncture site, displacement of sandbags, severe pain in the lower limbs, reduced skin temperature, or skin discoloration such as pallor or mottling, it is important to promptly inform medical personnel. 3. Daily Care. Except for patients with heart failure, postoperative patients can drink more water, generally between 1500 to 2000 ml, to promote the metabolism of the contrast agent. (2) Absolute prohibition of smoking and drinking, and consumption of a low-salt, low-fat, high-fiber diet. (3) Ensure smooth bowel movements; during the postoperative bed rest period, a bedpan should be used for urination and defecation. If there is constipation, a laxative can be used under the guidance of healthcare personnel. 4. Sports Management. In the early postoperative period, patients need to engage in appropriate activities under the guidance of medical staff, such as turning in bed and moving their lower limbs, to promote blood circulation and prevent deep vein thrombosis. Initially, light exercises like walking and jogging can be performed, gradually transitioning to aerobic activities like swimming and cycling. During exercise, heart rate should be monitored to remain within an appropriate range, avoiding excessive fatigue. 3. Discharge Education. (1) Follow the doctor's advice and take medication on time. Observe the blood circulation in the affected limb and pay attention to whether the distal parts of the lower limbs are cool, sensitive to cold, numb, sore, or if there are signs of intermittent claudication or other abnormal symptoms. You can check if the skin temperature of both lower limbs is consistent and assess whether the pulses of the femoral artery, popliteal artery, dorsalis pedis artery, and other arteries are normal. (2) Pay attention to any signs of bleeding, such as nosebleeds, gum bleeding, black stools, or unexplained bleeding spots or bruises on the skin. If any of these symptoms occur, medication should be stopped immediately and medical attention should be sought as soon as possible. (3) Keep your feet clean and dry. The water temperature for washing feet should not exceed 40°C, and the washing should last less than 10 minutes. Avoid vigorous rubbing to prevent skin abrasion. Pay attention to keeping the lower limbs warm and wear loose-fitting shoes. Avoid activities that may cause foot injuries, such as walking barefoot. After washing your feet daily, carefully check for any skin lesions. If any are found, seek medical attention as soon as possible and do not attempt to treat or trim them on your own. If there are ulcers or gangrene, keep the area clean and dry, avoid contact with water, and prevent the condition from worsening. (4) Regular outpatient follow-up. After vascular intervention, regular outpatient follow-up is required at one, three, six, and twelve months. If symptoms such as increased pain, movement difficulties, numbness, or cold limbs occur, seek medical attention promptly. If you have a stent in your body, please proactively inform the medical staff before any examinations to avoid any accidents.
© 2025 Health Tribe.


